444 Alaska Avenue
Suite #BAA205 Torrance, CA 90503 USA
+1 424 999 9627
24/7 Customer Support
sales@markwideresearch.com
Email us at
Suite #BAA205 Torrance, CA 90503 USA
24/7 Customer Support
Email us at
Corporate User License
Unlimited User Access, Post-Sale Support, Free Updates, Reports in English & Major Languages, and more
$3450
Market Overview
The back-end revenue cycle management market plays a crucial role in optimizing financial processes within the healthcare industry. This comprehensive guide explores the meaning, key insights, market dynamics, regional analysis, competitive landscape, segmentation, industry trends, and future outlook of this rapidly growing market. Additionally, we delve into the impact of COVID-19, key industry developments, and provide valuable suggestions for industry participants and stakeholders.
Meaning
Back-end revenue cycle management refers to the set of processes and strategies implemented by healthcare organizations to streamline and optimize financial operations. It encompasses various activities such as medical coding, billing, claims processing, payment reconciliation, denial management, and revenue analytics. By effectively managing the back-end revenue cycle, healthcare providers can enhance operational efficiency, reduce revenue leakage, improve cash flow, and achieve financial sustainability.
Executive Summary
The back-end revenue cycle management market has witnessed significant growth in recent years, driven by the increasing complexity of healthcare reimbursement systems, stringent regulations, rising healthcare costs, and the need for accurate and timely financial data. Healthcare organizations are increasingly realizing the importance of optimizing revenue cycle management to maximize revenue capture and minimize revenue leakage. This market analysis aims to provide key insights and strategic recommendations for stakeholders in the back-end revenue cycle management sector.
Important Note: The companies listed in the image above are for reference only. The final study will cover 18–20 key players in this market, and the list can be adjusted based on our client’s requirements.
Key Market Insights
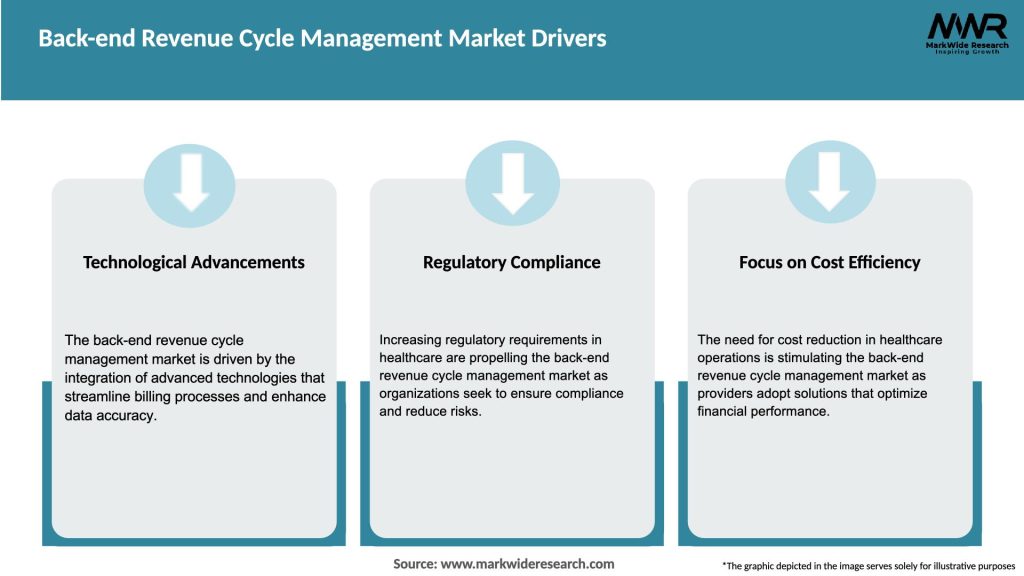
Market Drivers
Market Restraints
Market Opportunities
Market Dynamics
The back-end revenue cycle management market is characterized by intense competition among vendors, rapid technological advancements, and evolving regulatory landscapes. Key market dynamics include mergers and acquisitions, strategic partnerships, product launches, and innovations. Additionally, the market is influenced by shifting reimbursement models, evolving healthcare reforms, and the increasing focus on patient-centric care.
Regional Analysis
The back-end revenue cycle management market exhibits a significant presence across major regions, including North America, Europe, Asia Pacific, Latin America, and the Middle East and Africa. North America dominates the market due to the presence of well-established healthcare infrastructure, government initiatives for healthcare IT adoption, and a high focus on revenue cycle optimization. However, the Asia Pacific region is witnessing rapid growth, driven by increasing healthcare spending, expanding healthcare infrastructure, and the adoption of advanced technologies.
Competitive Landscape
Leading Companies in the Back-end Revenue Cycle Management Market:
Please note: This is a preliminary list; the final study will feature 18–20 leading companies in this market. The selection of companies in the final report can be customized based on our client’s specific requirements.
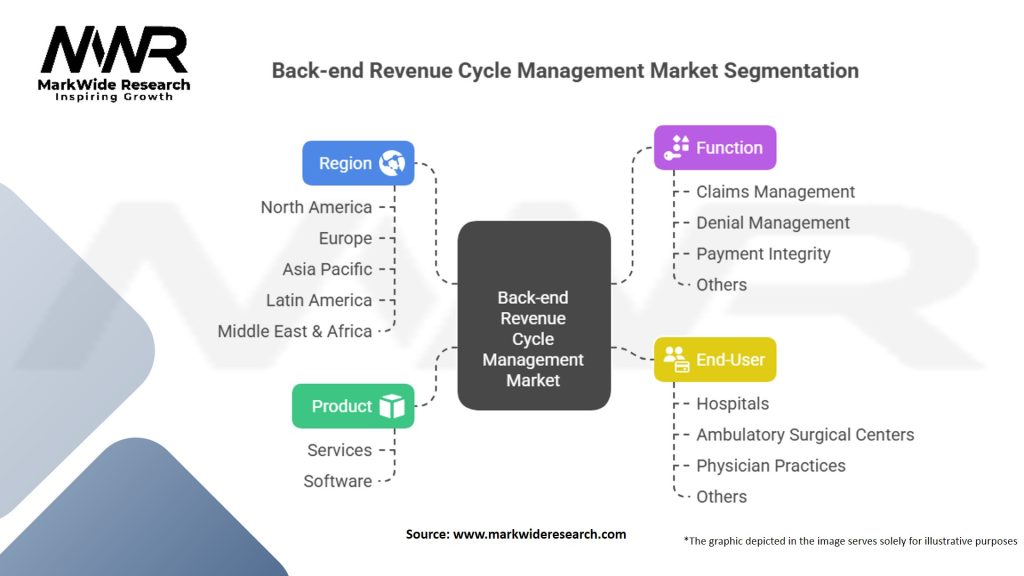
Segmentation The back-end revenue cycle management market can be segmented based on product type, delivery mode, end-user, and region. Product types include software solutions, outsourcing services, and consulting services. Delivery modes encompass on-premises, web-based, and cloud-based solutions. End-users of revenue cycle management solutions include hospitals, clinics, ambulatory surgical centers, and others.
Category-wise Insights
Key Benefits for Industry Participants and Stakeholders
SWOT Analysis Strengths:
Weaknesses:
Opportunities:
Threats:
Market Key Trends
COVID-19 Impact The COVID-19 pandemic has significantly impacted the back-end revenue cycle management market. Healthcare providers faced challenges such as reduced patient volumes, delayed reimbursements, and shifting payment models. However, the pandemic also accelerated the adoption of telehealth services, which created opportunities for revenue cycle management vendors. The focus on financial stability, operational efficiency, and accurate billing practices became even more critical during this period.
Key Industry Developments
Analyst Suggestions
Future Outlook
The back-end revenue cycle management market is expected to witness significant growth in the coming years. Factors such as increasing healthcare expenditure, evolving reimbursement models, the need for accurate financial data, and technological advancements will drive market expansion. The integration of AI, automation, and analytics will further optimize revenue cycle processes. Emerging markets and the expansion of telehealth services present lucrative opportunities for revenue cycle management vendors.
Conclusion
Efficient back-end revenue cycle management is crucial for healthcare organizations to optimize financial processes, improve revenue capture, and ensure long-term sustainability. This comprehensive guide provided insights into the market overview, meaning, key market insights, drivers, restraints, opportunities, dynamics, regional analysis, competitive landscape, segmentation, category-wise insights, benefits for stakeholders, SWOT analysis, market key trends, COVID-19 impact, industry developments, analyst suggestions, future outlook, and a conclusion. By adopting innovative solutions and best practices, stakeholders can navigate the evolving healthcare landscape and achieve financial success.
What is Back-end Revenue Cycle Management?
Back-end Revenue Cycle Management refers to the processes involved in managing the financial aspects of healthcare services after the patient has received care. This includes billing, collections, and claims management, ensuring that healthcare providers receive payment for their services efficiently.
What are the key players in the Back-end Revenue Cycle Management Market?
Key players in the Back-end Revenue Cycle Management Market include companies like Optum, Cerner Corporation, and McKesson Corporation, which provide various solutions for managing revenue cycles in healthcare settings, among others.
What are the main drivers of growth in the Back-end Revenue Cycle Management Market?
The growth of the Back-end Revenue Cycle Management Market is driven by the increasing complexity of healthcare billing, the need for improved cash flow management, and the rising adoption of electronic health records (EHR) systems that streamline revenue processes.
What challenges does the Back-end Revenue Cycle Management Market face?
Challenges in the Back-end Revenue Cycle Management Market include regulatory compliance issues, the high cost of technology implementation, and the need for skilled personnel to manage complex billing processes effectively.
What opportunities exist in the Back-end Revenue Cycle Management Market?
Opportunities in the Back-end Revenue Cycle Management Market include the integration of artificial intelligence for predictive analytics, the expansion of telehealth services, and the growing demand for outsourcing revenue cycle management to specialized firms.
What trends are shaping the Back-end Revenue Cycle Management Market?
Trends in the Back-end Revenue Cycle Management Market include the increasing use of automation to reduce manual errors, the shift towards value-based care models, and the emphasis on patient engagement to improve payment processes.
Back-end Revenue Cycle Management Market:
| Segmentation | Details |
|---|---|
| Product | Services, Software |
| Function | Claims Management, Denial Management, Payment Integrity, Others |
| End-User | Hospitals, Ambulatory Surgical Centers, Physician Practices, Others |
| Region | North America, Europe, Asia Pacific, Latin America, Middle East & Africa |
Please note: The segmentation can be entirely customized to align with our client’s needs.
Leading Companies in the Back-end Revenue Cycle Management Market:
Please note: This is a preliminary list; the final study will feature 18–20 leading companies in this market. The selection of companies in the final report can be customized based on our client’s specific requirements.
North America
o US
o Canada
o Mexico
Europe
o Germany
o Italy
o France
o UK
o Spain
o Denmark
o Sweden
o Austria
o Belgium
o Finland
o Turkey
o Poland
o Russia
o Greece
o Switzerland
o Netherlands
o Norway
o Portugal
o Rest of Europe
Asia Pacific
o China
o Japan
o India
o South Korea
o Indonesia
o Malaysia
o Kazakhstan
o Taiwan
o Vietnam
o Thailand
o Philippines
o Singapore
o Australia
o New Zealand
o Rest of Asia Pacific
South America
o Brazil
o Argentina
o Colombia
o Chile
o Peru
o Rest of South America
The Middle East & Africa
o Saudi Arabia
o UAE
o Qatar
o South Africa
o Israel
o Kuwait
o Oman
o North Africa
o West Africa
o Rest of MEA
Trusted by Global Leaders
Fortune 500 companies, SMEs, and top institutions rely on MWR’s insights to make informed decisions and drive growth.
ISO & IAF Certified
Our certifications reflect a commitment to accuracy, reliability, and high-quality market intelligence trusted worldwide.
Customized Insights
Every report is tailored to your business, offering actionable recommendations to boost growth and competitiveness.
Multi-Language Support
Final reports are delivered in English and major global languages including French, German, Spanish, Italian, Portuguese, Chinese, Japanese, Korean, Arabic, Russian, and more.
Unlimited User Access
Corporate License offers unrestricted access for your entire organization at no extra cost.
Free Company Inclusion
We add 3–4 extra companies of your choice for more relevant competitive analysis — free of charge.
Post-Sale Assistance
Dedicated account managers provide unlimited support, handling queries and customization even after delivery.
GET A FREE SAMPLE REPORT
This free sample study provides a complete overview of the report, including executive summary, market segments, competitive analysis, country level analysis and more.
ISO AND IAF CERTIFIED


GET A FREE SAMPLE REPORT
This free sample study provides a complete overview of the report, including executive summary, market segments, competitive analysis, country level analysis and more.
ISO AND IAF CERTIFIED


Suite #BAA205 Torrance, CA 90503 USA
24/7 Customer Support
Email us at