444 Alaska Avenue
Suite #BAA205 Torrance, CA 90503 USA
+1 424 999 9627
24/7 Customer Support
sales@markwideresearch.com
Email us at
Suite #BAA205 Torrance, CA 90503 USA
24/7 Customer Support
Email us at
Corporate User License
Unlimited User Access, Post-Sale Support, Free Updates, Reports in English & Major Languages, and more
$2450
Market Overview
The US Healthcare Payer Analytics market is a rapidly growing sector within the healthcare industry. With the increasing complexity of healthcare systems and the need for effective cost management, payers are turning to advanced analytics solutions to optimize their operations and improve decision-making. Payer analytics involves the collection, analysis, and interpretation of data related to healthcare claims, patient behavior, provider performance, and other relevant factors. These insights help payers identify trends, assess risks, streamline processes, and enhance the overall quality and efficiency of healthcare services.
Meaning
Healthcare payer analytics refers to the use of data analysis techniques and tools to gain valuable insights into various aspects of payer operations. It involves the examination of vast amounts of data from multiple sources, such as claims data, electronic health records, pharmacy records, and demographic information. By applying advanced analytics algorithms and models, payers can uncover patterns, correlations, and trends in the data, enabling them to make data-driven decisions and improve their business outcomes.
Executive Summary
The US Healthcare Payer Analytics market is witnessing significant growth due to the rising demand for cost-effective and high-quality healthcare services. Payers are increasingly adopting analytics solutions to better understand their members, manage risk, optimize network utilization, and identify opportunities for cost containment. The market is characterized by the presence of numerous vendors offering a wide range of analytics tools and platforms tailored to the specific needs of payers.
Important Note: The companies listed in the image above are for reference only. The final study will cover 18–20 key players in this market, and the list can be adjusted based on our client’s requirements.
Key Market Insights
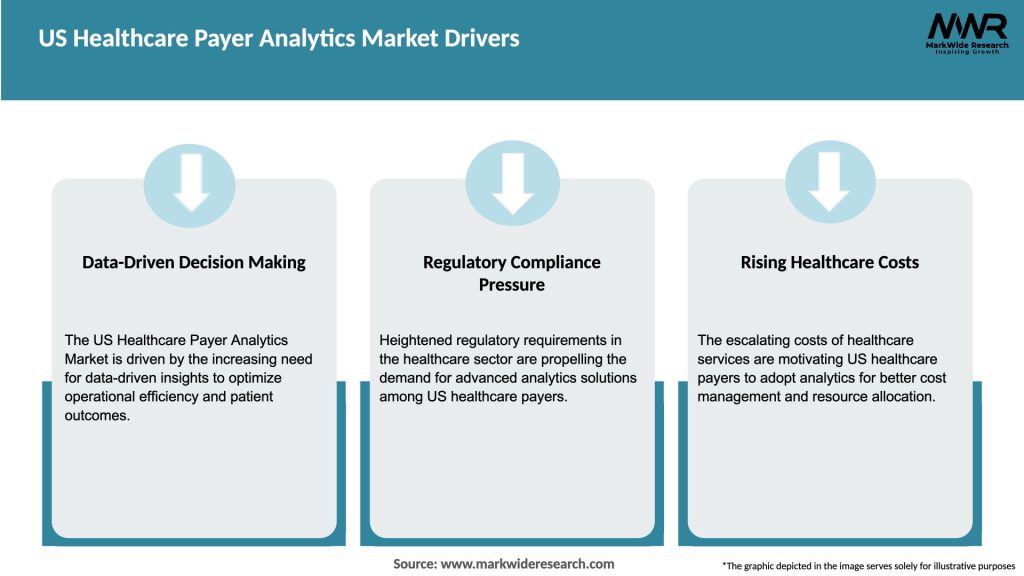
Market Drivers
Market Restraints
Market Opportunities

Market Dynamics
The US Healthcare Payer Analytics market is characterized by intense competition among vendors, with continuous advancements in analytics capabilities. Payers are increasingly looking for comprehensive analytics solutions that can provide actionable insights across multiple areas, such as claims processing, provider performance evaluation, fraud detection, and member management. Additionally, the market is witnessing partnerships and collaborations between analytics solution providers and healthcare organizations to leverage combined expertise and deliver innovative solutions.
Regional Analysis
The US Healthcare Payer Analytics market exhibits a strong presence across all regions of the country. However, certain regions, such as California, New York, and Texas, have emerged as major hubs for healthcare innovation, attracting numerous analytics vendors and fostering a conducive environment for market growth. Factors such as population demographics, healthcare infrastructure, and regulatory policies play a significant role in shaping regional dynamics and adoption of payer analytics solutions.
Competitive Landscape
Leading Companies in the US Healthcare Payer Analytics Market:
Please note: This is a preliminary list; the final study will feature 18–20 leading companies in this market. The selection of companies in the final report can be customized based on our client’s specific requirements.
Segmentation
The US Healthcare Payer Analytics market can be segmented based on:
Category-wise Insights
Key Benefits for Industry Participants and Stakeholders
SWOT Analysis
Strengths:
Weaknesses:
Opportunities:
Threats:
Market Key Trends
Covid-19 Impact
The COVID-19 pandemic has significantly influenced the US Healthcare Payer Analytics market. The pandemic highlighted the importance of accurate data analysis and predictive modeling in managing public health crises. Payers have leveraged analytics solutions to track the spread of the virus, identify high-risk populations, and allocate resources efficiently. Additionally, the pandemic accelerated the adoption of telehealth services, leading to increased demand for analytics solutions to monitor telehealth utilization, assess the quality of virtual care, and ensure equitable access to healthcare services.
Key Industry Developments
Analyst Suggestions
Future Outlook
The US Healthcare Payer Analytics market is expected to witness sustained growth in the coming years. Payers will continue to invest in analytics solutions to navigate the evolving healthcare landscape, address rising costs, and deliver high-quality, value-based care. Advancements in AI, ML, and natural language processing will further enhance the capabilities of payer analytics, enabling more accurate predictions, personalized interventions, and improved patient outcomes. The integration of payer analytics with emerging technologies, such as telehealth and wearable devices, will open new opportunities for data-driven decision-making and proactive healthcare management.
Conclusion
The US Healthcare Payer Analytics market is experiencing significant growth as payers recognize the value of data-driven insights in optimizing operations, improving decision-making, and enhancing the overall quality of healthcare services. The adoption of analytics solutions enables payers to manage risks, reduce costs, combat fraud, and deliver personalized care to their members. However, challenges related to data privacy, skilled workforce availability, and data integration need to be addressed to fully harness the potential of payer analytics. With advancements in technology and a focus on innovation, payer analytics is poised to play a crucial role in shaping the future of healthcare delivery in the United States.
What is US Healthcare Payer Analytics?
US Healthcare Payer Analytics refers to the systematic analysis of data related to healthcare payers, including insurance companies and government programs, to improve decision-making, operational efficiency, and patient outcomes.
Who are the key players in the US Healthcare Payer Analytics Market?
Key players in the US Healthcare Payer Analytics Market include Optum, IBM Watson Health, Cerner Corporation, and McKesson Corporation, among others.
What are the main drivers of growth in the US Healthcare Payer Analytics Market?
The main drivers of growth in the US Healthcare Payer Analytics Market include the increasing demand for data-driven decision-making, the rise in healthcare costs, and the need for improved patient care and operational efficiency.
What challenges does the US Healthcare Payer Analytics Market face?
Challenges in the US Healthcare Payer Analytics Market include data privacy concerns, the complexity of integrating diverse data sources, and the need for skilled professionals to interpret analytics effectively.
What opportunities exist in the US Healthcare Payer Analytics Market?
Opportunities in the US Healthcare Payer Analytics Market include advancements in artificial intelligence and machine learning, the growing emphasis on value-based care, and the potential for personalized medicine through data insights.
What trends are shaping the US Healthcare Payer Analytics Market?
Trends shaping the US Healthcare Payer Analytics Market include the increasing use of predictive analytics, the integration of real-time data for better decision-making, and the shift towards patient-centric care models.
US Healthcare Payer Analytics Market
| Segmentation Details | Information |
|---|---|
| Component | Software, Services |
| Application | Fraud Detection, Revenue Cycle Management, Risk Adjustment & Assessment, Others |
| End User | Private Payers, Public Payers |
| Region | United States |
Please note: The segmentation can be entirely customized to align with our client’s needs.
Leading Companies in the US Healthcare Payer Analytics Market:
Please note: This is a preliminary list; the final study will feature 18–20 leading companies in this market. The selection of companies in the final report can be customized based on our client’s specific requirements.
Trusted by Global Leaders
Fortune 500 companies, SMEs, and top institutions rely on MWR’s insights to make informed decisions and drive growth.
ISO & IAF Certified
Our certifications reflect a commitment to accuracy, reliability, and high-quality market intelligence trusted worldwide.
Customized Insights
Every report is tailored to your business, offering actionable recommendations to boost growth and competitiveness.
Multi-Language Support
Final reports are delivered in English and major global languages including French, German, Spanish, Italian, Portuguese, Chinese, Japanese, Korean, Arabic, Russian, and more.
Unlimited User Access
Corporate License offers unrestricted access for your entire organization at no extra cost.
Free Company Inclusion
We add 3–4 extra companies of your choice for more relevant competitive analysis — free of charge.
Post-Sale Assistance
Dedicated account managers provide unlimited support, handling queries and customization even after delivery.
GET A FREE SAMPLE REPORT
This free sample study provides a complete overview of the report, including executive summary, market segments, competitive analysis, country level analysis and more.
ISO AND IAF CERTIFIED


GET A FREE SAMPLE REPORT
This free sample study provides a complete overview of the report, including executive summary, market segments, competitive analysis, country level analysis and more.
ISO AND IAF CERTIFIED


Suite #BAA205 Torrance, CA 90503 USA
24/7 Customer Support
Email us at