444 Alaska Avenue
Suite #BAA205 Torrance, CA 90503 USA
+1 424 999 9627
24/7 Customer Support
sales@markwideresearch.com
Email us at
Suite #BAA205 Torrance, CA 90503 USA
24/7 Customer Support
Email us at
Corporate User License
Unlimited User Access, Post-Sale Support, Free Updates, Reports in English & Major Languages, and more
$3450
Market Overview
The global Urology Ultrasound market is experiencing steady growth, driven by the rising prevalence of urological disorders, the shift toward non-invasive diagnostic modalities, and continuous technological advancements in ultrasound imaging. Urology ultrasound systems—ranging from portable point-of-care devices to high-end cart-based platforms—are used for the diagnosis, monitoring, and interventional guidance of conditions affecting the urinary tract, kidneys, bladder, prostate, and male reproductive organs. With an aging population, increasing incidence of kidney stones, urinary incontinence, benign prostatic hyperplasia (BPH), and prostate cancer, clinicians are turning to ultrasound for its safety profile (no ionizing radiation), real-time imaging capability, and cost-effectiveness compared to CT or MRI. Expansion of ambulatory care facilities, point-of-care ultrasound (POCUS) adoption, and telemedicine integration are further broadening access to urology ultrasound across hospital, clinic, and remote settings.
Meaning
Urology ultrasound refers to the use of high-frequency sound waves to create images of the urogenital system. A transducer emits and receives acoustic signals that reflect off tissues, producing grayscale, Doppler, and elastography images. In urology applications, transducers may be placed transabdominally, transrectally, or endoluminally. Transrectal ultrasound (TRUS) is the standard for prostate imaging and biopsy guidance. Doppler ultrasound evaluates blood flow to assess renal perfusion or vascular abnormalities. Elastography measures tissue stiffness, aiding in differentiating benign from malignant lesions in the prostate or testes. Innovations such as contrast-enhanced ultrasound (CEUS) and fusion imaging (overlaying ultrasound on CT/MRI) enhance lesion characterization and interventional accuracy.
Executive Summary
The Urology Ultrasound market is projected to grow at a compound annual growth rate (CAGR) of 6–8% through 2030. Growth is underpinned by demographic shifts toward older age groups, increased screening for prostate cancer, rising incidence of renal disease and urinary tract stones, and the expansion of minimally invasive interventional procedures. Market leaders are investing in 3D/4D imaging, AI-driven lesion detection, and handheld ultrasound devices optimized for urology. Regulatory approvals of contrast agents for ultrasound, growing reimbursement for TRUS-guided biopsies, and tele-ultrasound platforms enabling remote expert consultation are accelerating adoption. Key stakeholders—including hospitals, specialty urology clinics, imaging centers, and OEMs—are focusing on comprehensive service contracts and training to maximize system utilization and patient throughput.
Important Note: The companies listed in the image above are for reference only. The final study will cover 18–20 key players in this market, and the list can be adjusted based on our client’s requirements.
Key Market Insights
Rising Disease Burden: Global prevalence of prostate cancer—second most common cancer in men—and kidney stones is fueling demand for diagnostic and interventional ultrasound.
Modalities Expansion: Elastography and CEUS are emerging as valuable tools in differentiating benign versus malignant lesions and monitoring fibrosis in transplant kidneys.
Point-of-Care Growth: The POCUS segment is growing rapidly as urologists and primary care providers adopt portable ultrasound to streamline workflow and improve bedside diagnostics.
AI Integration: Machine-learning algorithms for automated prostate volume measurement, kidney stone detection, and Doppler flow quantification are reducing operator variability and exam times.
Telemedicine Enablement: Cloud-based image sharing and remote guidance platforms allow specialists to support exams in underserved regions and rural clinics, enhancing access to urology expertise.
Market Drivers
Several factors are driving growth in the Urology Ultrasound market:
Demographic Trends: Aging populations in North America, Europe, and Asia-Pacific increase the incidence of urologic conditions requiring imaging for diagnosis and treatment monitoring.
Preference for Non-Invasive Diagnostics: Ultrasound’s safety profile without ionizing radiation makes it preferable for repeated imaging in chronic kidney disease and prostate cancer surveillance.
Technological Innovation: Advances in probe design (e.g., high-frequency linear transducers), software (3D/4D reconstruction, elastography), and form factors (handheld, tablet-based systems) expand clinical applications.
Minimally Invasive Interventions: Ultrasound guidance for percutaneous nephrolithotomy, renal biopsies, prostate brachytherapy, and focal ablation therapies improves procedural accuracy and reduces complications.
Healthcare Infrastructure Development: Investment in ambulatory surgery centers and outpatient clinics boosts demand for compact, cost-effective ultrasound systems optimized for urology workflows.
Market Restraints
Despite positive trends, the market faces several challenges:
Operator Dependency: Ultrasound image quality and diagnostic accuracy are highly dependent on the skill and experience of the operator, limiting standardization.
Cost Constraints: High-end systems with 3D/4D and CEUS capabilities carry premium prices, presenting budgetary hurdles for smaller clinics and emerging markets.
Alternate Modalities: CT and MRI offer superior spatial resolution and tissue contrast for certain urologic applications (e.g., complex stone mapping, soft-tissue characterization), competing with ultrasound.
Reimbursement Variability: Differences in coverage for ultrasound procedures—especially CEUS—across countries and payers can impact utilization rates.
Regulatory Hurdles: Approval processes for novel ultrasound applications (e.g., targeted microbubble contrast agents) can be lengthy and costly, slowing market rollout.
Market Opportunities
The Urology Ultrasound market presents several growth opportunities:
Elastography Adoption: Expanding use of shear-wave and strain elastography for prostate cancer grading, transplant kidney fibrosis staging, and differentiating scrotal masses.
Contrast-Enhanced Ultrasound (CEUS): New indications and contrast agents for renal lesion characterization and microvascular imaging in prostate and bladder tumors.
Fusion Imaging: Integration of real-time ultrasound with pre-acquired CT/MRI datasets enhances biopsy accuracy and targeted focal therapy planning.
AI-Driven Tools: Development of automated workflows—such as kidney segmentation, stone detection, and prostate ROI cropping—reduces exam time and inter-observer variability.
Handheld Devices: Rapidly growing segment of handheld and wireless ultrasound platforms, enabling urologists to perform point-of-care exams in office settings, remote clinics, and even at home for telehealth initiatives.
Market Dynamics
Consolidation and Partnerships: OEMs are partnering with software startups and academic institutions to co-develop AI algorithms and contrast agents.
Training and Education: Increased focus on standardized curricula and certifications for urologic ultrasound to mitigate operator dependency and improve image reproducibility.
Service Models: OEMs offer subscription and pay-per-use models for advanced features (e.g., CEUS, elastography) to lower entry barriers for smaller practices.
Global Expansion: Strategic initiatives to enter emerging markets—Latin America, Middle East & Africa—via local partnerships and tailored low-cost system variants.
Regulatory Evolution: Harmonization of ultrasound device standards (e.g., IEC, FDA guidance) and expedited pathways for AI-based software as a medical device (SaMD) facilitate innovation.
Regional Analysis
North America: Largest regional market driven by high adoption of advanced imaging modalities, strong reimbursement environment, and widespread use of TRUS in prostate cancer management.
Europe: Significant growth in Western Europe with robust healthcare infrastructure; Eastern Europe emerging as a high-growth region as ultrasound access expands.
Asia-Pacific: Fastest-growing region, led by China and India, where rising healthcare spending, urologic procedural volumes, and rural telemedicine initiatives accelerate adoption of cost-effective and portable ultrasound solutions.
Latin America: Moderate growth supported by private healthcare investments and increasing urologic service offerings in urban centers of Brazil, Mexico, and Argentina.
Middle East & Africa: Nascent market with growing uptake in GCC countries; government-led healthcare modernization and telemedicine projects are key growth drivers.
Competitive Landscape
Leading Companies in the Urology Ultrasound Market:
Please note: This is a preliminary list; the final study will feature 18–20 leading companies in this market. The selection of companies in the final report can be customized based on our client’s specific requirements.
Segmentation
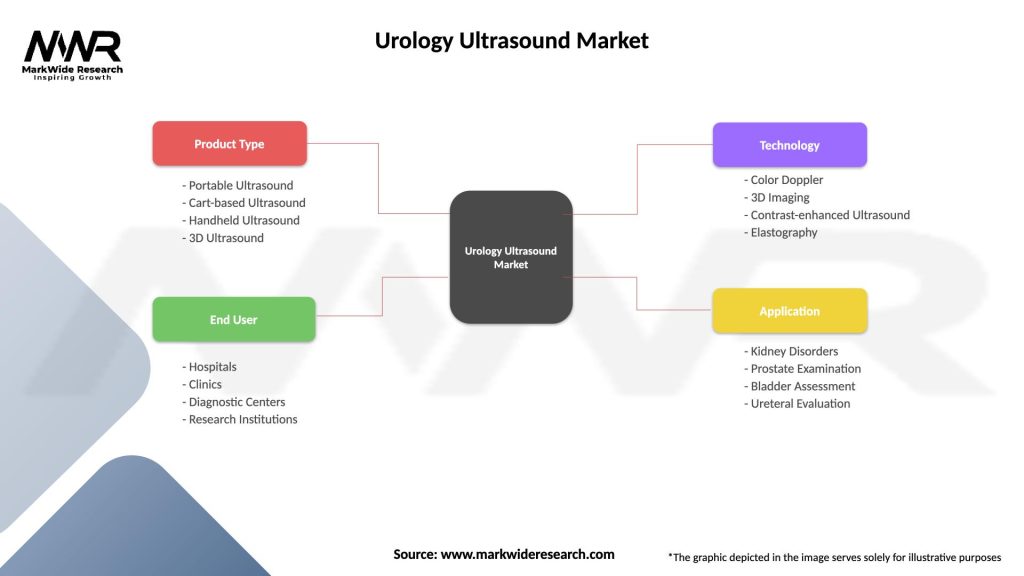
By Product: Cart-Based Ultrasound Systems, Portable/Handheld Ultrasound Devices, Contrast Agents, AI-Driven Software, Elastography Modules.
By Modality: 2D Grayscale, Doppler (Color, Power, Spectral), 3D/4D Imaging, Elastography, CEUS.
By Application: Prostate Imaging & Biopsy Guidance, Renal Tract Evaluation, Bladder Function Studies, Testicular & Scrotal Imaging, Interventional Urology (needling, ablation).
By End User: Hospitals, Urology Clinics, Diagnostic Imaging Centers, Academic & Research Institutes, Ambulatory Surgery Centers.
By Region: North America, Europe, Asia-Pacific, Latin America, Middle East & Africa.
Category-wise Insights
Cart-Based Systems: Feature-rich platforms with high-end transducers, AI analytics for automated measurements (prostate volume, post-void residual), and connectivity for PACS integration—dominate large hospital settings.
Portable/Handheld Devices: Battery-powered, lightweight devices ideal for POCUS, office-based urology practices, and remote clinics; feature intuitive touchscreen interfaces and secure cloud connectivity.
Elastography Modules: Shear-wave and strain elastography add-ons provide quantitative stiffness maps and fibrosis scores, improving lesion characterization in prostate and kidney applications.
CEUS: Contrast protocols using microbubble agents enhance vascular imaging of small renal masses and prostatic nodules, enabling better differentiation of benign versus malignant lesions.
AI-Driven Software: Automated image optimization, organ segmentation, and lesion detection tools reduce exam time, standardize reporting, and support decision-making in urologic diagnostics.
Key Benefits for Industry Participants and Stakeholders
Improved Diagnostic Confidence: Advanced imaging modalities (elastography, CEUS) and AI tools increase sensitivity and specificity for early detection of urologic cancers and nephrolithiasis.
Workflow Efficiency: Automated measurements and predefined urology presets streamline exams, enabling higher patient throughput and reduced operator variability.
Enhanced Patient Experience: Non-invasive, radiation-free imaging promotes patient safety and compliance with surveillance protocols for chronic urologic conditions.
Expanded Access: Portable and tele-ultrasound solutions extend urologic imaging services to outpatient clinics, rural hospitals, and home-based care models.
Interventional Guidance: Real-time ultrasound guidance for biopsies, drainage procedures, and ablation therapies improves procedure accuracy and reduces complication rates.
SWOT Analysis
Strengths:
Versatility of ultrasound across diagnostic and interventional urology applications.
Strong safety profile with no ionizing radiation exposure.
Continuous innovation in AI and contrast technologies enhancing clinical utility.
Weaknesses:
Significant operator dependency affecting image quality and diagnostic accuracy.
High upfront costs for advanced 3D/4D and CEUS-enabled systems.
Reimbursement variability for novel ultrasound applications (e.g., elastography, CEUS).
Opportunities:
Expansion of point-of-care and handheld ultrasound use by urologists and primary care providers.
Growth of AI-based decision support tools to augment diagnostic workflows and reduce learning curves.
Development of disease-specific contrast agents and microbubbles for targeted molecular imaging in urology.
Threats:
Competition from cross-sectional modalities (CT, MRI) offering higher anatomical detail in complex cases.
Regulatory and reimbursement challenges for emerging applications like CEUS and targeted microbubble imaging.
Potential supply chain disruptions for specialized probes and contrast agents.
Market Key Trends
AI-Driven Diagnostics: Adoption of deep-learning algorithms for automated prostate segmentation, kidney lesion classification, and bladder wall thickness quantification.
Fusion Imaging: Real-time overlay of ultrasound with MRI/CT data enhances biopsy targeting and treatment planning for focal therapy in prostate cancer.
Miniaturization: Development of pocket-sized ultrasound probes and wireless transducers for rapid bedside and remote examinations.
Contrast Innovations: Investigation of targeted microbubble agents binding to PSMA and VEGF receptors opens the door to molecular ultrasound imaging in urology.
Cloud-Based Collaboration: Secure image sharing and tele-ultrasound platforms enable multidisciplinary consultations and expert review across geographic boundaries.
Covid-19 Impact
The Covid-19 pandemic accelerated the adoption of portable and tele-ultrasound solutions to minimize patient movement and reduce infection risk. Urology practices adopted handheld devices for preliminary assessments, reducing dependence on centralized imaging suites. PPE requirements and social distancing mandates prompted workflow redesigns in imaging departments, with emphasis on rapid disinfectable probe designs and exam protocols to optimize throughput while ensuring safety.
Key Industry Developments
Philips EPIQ Elite Release: Introduced enhanced AI-driven urology suite with automated prostate segmentation and 3D biopsy planning tools.
GE Healthcare’s Vscan Air: Launched wireless, pocket-sized ultrasound probe integrated with tablet app, expanding POCUS use in urology clinics and remote screening programs.
Samsung RS85 Prestige Upgrade: Added ARFI shear-wave elastography and CEUS capabilities optimized for renal lesion characterization and prostate stiffness mapping.
Analyst Suggestions
Invest in Training Programs: Develop comprehensive urology-specific ultrasound curricula—combining hands-on workshops, simulation, and digital modules—to reduce operator dependency and improve diagnostic consistency.
Expand Reimbursement Coverage: Engage with payers and policymakers to demonstrate clinical and economic benefits of advanced ultrasound applications (elastography, CEUS) and secure favorable reimbursement codes.
Foster Collaborative Ecosystems: Partner with software and AI startups, contrast-agent developers, and academic research centers to co-develop integrated solutions tailored to urology workflows.
Optimize Service Models: Offer modular service contracts and pay-per-use subscriptions for advanced imaging features to lower entry barriers for smaller practices and emerging markets.
Future Outlook
The Urology Ultrasound market is poised for sustained growth as technological innovation, demographic pressures, and healthcare delivery transformations converge. AI-driven automation will become ubiquitous, standardizing exams and accelerating diagnosis. Emerging molecular ultrasound techniques using targeted contrast agents will open new frontiers in early cancer detection and personalized therapy monitoring. Point-of-care and tele-ultrasound platforms will democratize access to urology imaging, particularly in underserved and remote regions. As value-based care models gain traction, ultrasound’s favorable safety, cost, and workflow profile will solidify its role as the cornerstone imaging modality in urology.
Conclusion
In conclusion, the Urology Ultrasound market represents a dynamic intersection of demographic need, technological innovation, and healthcare delivery evolution. Stakeholders—from OEMs and software developers to clinicians and health systems—stand to benefit by embracing AI, contrast-enhanced, and fusion imaging solutions that enhance diagnostic accuracy, procedural guidance, and patient outcomes. By investing in training, expanding access via portable and tele-ultrasound, and securing supportive reimbursement frameworks, the industry can fully realize ultrasound’s potential to transform urologic care worldwide.
What is Urology Ultrasound?
Urology Ultrasound refers to the use of ultrasound technology in the field of urology to diagnose and monitor conditions related to the urinary tract and male reproductive organs. This non-invasive imaging technique helps in assessing kidney stones, bladder issues, and prostate health, among other applications.
What are the key players in the Urology Ultrasound Market?
Key players in the Urology Ultrasound Market include Siemens Healthineers, GE Healthcare, Philips Healthcare, and Canon Medical Systems, among others. These companies are known for their innovative ultrasound technologies and solutions tailored for urological applications.
What are the growth factors driving the Urology Ultrasound Market?
The Urology Ultrasound Market is driven by factors such as the increasing prevalence of urological disorders, advancements in ultrasound technology, and the growing demand for non-invasive diagnostic procedures. Additionally, the rising awareness of early diagnosis and treatment options contributes to market growth.
What challenges does the Urology Ultrasound Market face?
Challenges in the Urology Ultrasound Market include the high cost of advanced ultrasound systems and the need for skilled professionals to operate these devices. Furthermore, competition from alternative imaging modalities may hinder market expansion.
What opportunities exist in the Urology Ultrasound Market?
Opportunities in the Urology Ultrasound Market include the development of portable ultrasound devices and the integration of artificial intelligence for enhanced diagnostic accuracy. Additionally, expanding healthcare infrastructure in emerging markets presents significant growth potential.
What trends are shaping the Urology Ultrasound Market?
Trends in the Urology Ultrasound Market include the increasing adoption of point-of-care ultrasound and the use of telemedicine for remote consultations. Moreover, innovations in imaging technology, such as three-dimensional ultrasound, are enhancing diagnostic capabilities.
Urology Ultrasound Market
| Segmentation Details | Description |
|---|---|
| Product Type | Portable Ultrasound, Cart-based Ultrasound, Handheld Ultrasound, 3D Ultrasound |
| End User | Hospitals, Clinics, Diagnostic Centers, Research Institutions |
| Technology | Color Doppler, 3D Imaging, Contrast-enhanced Ultrasound, Elastography |
| Application | Kidney Disorders, Prostate Examination, Bladder Assessment, Ureteral Evaluation |
Please note: The segmentation can be entirely customized to align with our client’s needs.
Leading Companies in the Urology Ultrasound Market:
Please note: This is a preliminary list; the final study will feature 18–20 leading companies in this market. The selection of companies in the final report can be customized based on our client’s specific requirements.
North America
o US
o Canada
o Mexico
Europe
o Germany
o Italy
o France
o UK
o Spain
o Denmark
o Sweden
o Austria
o Belgium
o Finland
o Turkey
o Poland
o Russia
o Greece
o Switzerland
o Netherlands
o Norway
o Portugal
o Rest of Europe
Asia Pacific
o China
o Japan
o India
o South Korea
o Indonesia
o Malaysia
o Kazakhstan
o Taiwan
o Vietnam
o Thailand
o Philippines
o Singapore
o Australia
o New Zealand
o Rest of Asia Pacific
South America
o Brazil
o Argentina
o Colombia
o Chile
o Peru
o Rest of South America
The Middle East & Africa
o Saudi Arabia
o UAE
o Qatar
o South Africa
o Israel
o Kuwait
o Oman
o North Africa
o West Africa
o Rest of MEA
Trusted by Global Leaders
Fortune 500 companies, SMEs, and top institutions rely on MWR’s insights to make informed decisions and drive growth.
ISO & IAF Certified
Our certifications reflect a commitment to accuracy, reliability, and high-quality market intelligence trusted worldwide.
Customized Insights
Every report is tailored to your business, offering actionable recommendations to boost growth and competitiveness.
Multi-Language Support
Final reports are delivered in English and major global languages including French, German, Spanish, Italian, Portuguese, Chinese, Japanese, Korean, Arabic, Russian, and more.
Unlimited User Access
Corporate License offers unrestricted access for your entire organization at no extra cost.
Free Company Inclusion
We add 3–4 extra companies of your choice for more relevant competitive analysis — free of charge.
Post-Sale Assistance
Dedicated account managers provide unlimited support, handling queries and customization even after delivery.
GET A FREE SAMPLE REPORT
This free sample study provides a complete overview of the report, including executive summary, market segments, competitive analysis, country level analysis and more.
ISO AND IAF CERTIFIED


GET A FREE SAMPLE REPORT
This free sample study provides a complete overview of the report, including executive summary, market segments, competitive analysis, country level analysis and more.
ISO AND IAF CERTIFIED


Suite #BAA205 Torrance, CA 90503 USA
24/7 Customer Support
Email us at